Nursing the Future
Brenau University uses technology not only to teach future nurses skills and procedures but also as tools for helping them learn how to interact with other human beings – especially their patients.
By James Swift
Mark Maverick suffers intense chest pains and shortness of breath. The 67-year-old veteran’s toenails and fingernails turn blue. Medical personnel surround him. They work in an astonishingly well-organized fashion, darting in and out of the room at Brenau Hospital. Nurse Kelly Wright rapidly scrawls updates on the patient’s condition on a whiteboard. Nurse Melissa McDowell phones in vital information to treatment specialist Jane Anderson-Buffington.
Their diagnosis for the patient’s respiratory problems: a side effect of cardiomyopathy, a disease affecting muscles in the heart.
Nurse Kathy Bridgefarmer immediately places an oxygen mask on Maverick’s face, and Anderson-Buffington swoops in to administer the lifesaving medication. Because of precisely coordinated teamwork, the patient stabilizes, and it appears he will survive the evening.
Then, a member of the Brenau nursing school staff flips a switch, and Mark Maverick’s vital signs cease.
Don’t worry. Maverick did not die because he literally never lived. He was not an actual critically ill patient. He just played one in a training exercise for Brenau nursing school faculty and staff in its human simulator laboratory in Gainesville, Georgia. Nor is Brenau Hospital an actual medical facility. He merely existed as the persona affixed to a $68,000 piece of machinery posing as a critically ill patient in a hospital emergency room.
Thanks to a significant contribution several years ago by Gainesville residents Anne and George Thomas, the nursing school in 2008 established one of the first human simulator centers among nursing schools in the United States. Simulators mimic virtually any human condition nurses are likely to encounter with real hospital patients. They breathe, blink, bleed and bellows loud cries. From interacting with them, students learn quick-thinking patient care skills as well as teamwork and managing the sometimes overwhelming pressures of a medical career.
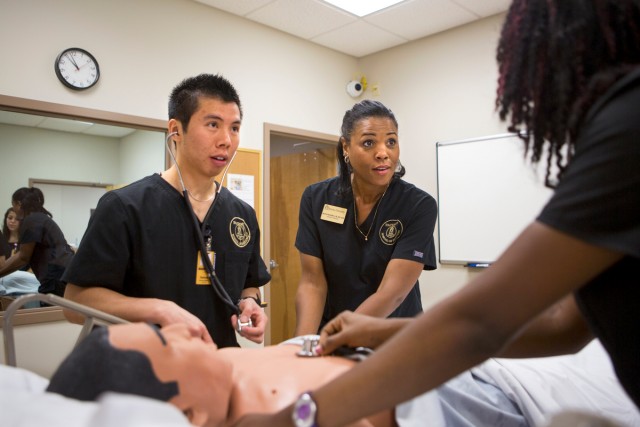
A new way to learn
Since the acquisition of that first CAE Healthcare iStan patient simulator, Brenau acquired a second iStan (each of them can pose as either male or female patients) plus a $46,000 PediaSim ECS male child model and, most recently, a $4,000 newborn infant birthing simulator. They all reside in a small hospital-like suite in the nursing school at the Brenau East campus in Gainesville. It costs about $24,000 a year for maintenance and supplies to keep them all in shape – not counting personnel who run the lab and oversee student work there.
What you witnessed in that earlier scenario was Brenau nursing faculty members who train themselves to use the lab before they put their students through it. However, faculty, staff and students in the Brenau School of Nursing who participated in the recent training exercise that kept Mark alive worked just as diligently in that manufactured, fast-paced mock-up of a hospital clinical environment with the manufactured patient as if they had been in a real hospital environment with a human being on the gurney. Sure, such drills ingrain in students the skills and technical procedures they will need so they can operate almost by rote in emergency situations. However, they also learn the importance of cooperation with one another and get a feel for dealing with patients in every emotional and medical state and how to manage the sometimes overwhelming pressures and day-to-day stress of medical careers.
The nursing school, which now offers undergraduate through doctorate degrees in Gainesville and at the North Atlanta/ Norcross campus (with an eye toward a future nursing program in Jacksonville, Florida), has some lofty goals for expansion, some of which are addressed in the university’s $40 million ForeverGold comprehensive campaign. The $12.5 million health care and sciences initiative addresses development of Brenau Downtown Center as an integrated health sciences facility, expansion of rehabilitative sciences programs, and enhancement on nursing education. The latter includes goals for funding a broader role for human simulators in health professions training, as well as establishing another kind of patient simulation training – a Standardized Patient Program that enables students to work with trained actors who pose as patients.
“Nurses represent the largest segment of health care professionals in the United States, yet, nationwide, we are experiencing a critical shortage of nurses,” said President Ed Schrader. “Because of technologies like the simulators, Brenau can successfully prepare our students with real-world experience. So it is imperative that we continue providing advanced technology to support instruction in all of our professional degree programs.”
Life-or-death consequences
School of Nursing Director Dina Hewett says the simulations are invaluable, as they enable students to experience things they are unlikely go through in clinical training, like treating a patient with congestive heart failure.
“We like to compare it to flight simulators,” she says. “Our human simulators can provide a similar experience for our nursing students. They can basically crash the plane in a safe environment, learn from that and go back and do it again.”
Operators control the extraordinarily lifelike mannequins from a windowed control room via a wireless connection. The computer for each mock hospital room operates special software that manipulates the heartbeat, breathing and urinary tracts of the simulators. There’s even an audio system installed in their larynxes so that role-players behind the scenes can dub in their own lines of dialogue to tell the students where it hurts or answer their questions.
Simulators, which weigh about the same as six-foot adult male who has to be horsed around in a hospital bed often by a much smaller nurse, can replicate everything from drug-induced heart attacks to automobile-accident-spawned trauma. To give the experience a heightened sense of realism, staff and faculty often mix in some fake blood and guts as well. From bleeding on a nurse’s clean scrubs to in-the-bed bladder incontinence, the simulators can do just about anything a human patient might do.
Even die.
“It’s a little intimidating at first, but students love it,” say Jane Anderson-Buffington, an assistant professor who teaches senior-level nursing courses. “Once the simulator starts blinking his eyes and talking, students realize it is a very realistic situation.” The lab is where the proverbial rubber hits the road. Students really begin to think critically about the profession and how successful in it they’re likely to be.
The best kind of practice
Thomas Doyle, president and CEO of SimOne Healthcare Consultants in St. Petersburg, Florida, says many universities and colleges once considered the devices novelties, if not outright wastes of money. Today, however, he says more and more nursing programs across the country are clamoring for the same technology Brenau has had for almost a decade.
“Fifteen years ago, people said to me ‘why do we need to do this?’” he says. “Now, it’s ‘How can we do more?’”
As a former health care provider, Doyle knows all too well how serious medical mistakes can be. He recalled a time when he, as a staff nurse at the Henry Ford Hospital in Detroit, treated a patient who sustained multiple trauma and a head injury in an automobile accident. He watched her die after he gave her 12 milligrams of a medication when the correct dosage was just 0.12 milligrams, a hundred times less.
That incident weighed heavily on his mind throughout the rest of his nursing career. It was a major factor in his decision to enter the emerging patient simulator industry in 1997 to help prepare nurses better to reduce the risk that they would make similar life-and-death mistakes in their careers.
Beyond building critical thinking skills, the simulators also give students a safe venue to make those kinds of miscalculations as well as witness their grave consequences without actually losing a patient, he says.
“In the sim center, we can allow them to make mistakes,” he says, “and they can see firsthand the outcomes of their actions.”
An increasingly vital tool
A growing body of research indicates the simulators are just as efficient in training students as tried-and-true hospital clinicals. Last year, the National Council of State Boards of Nursing published the results of a longitudinal study examining the effectiveness of simulation training compared to traditional clinicals in pre-licensed nursing education programs. According to their findings, as much as 50 percent of clinical experiences could be replaced by simulations comparable to the ones used at Brenau, with virtually no impact on National Council Licensure Examination pass rates.
Melissa McDowell, an assistant professor who primarily works alongside junior nursing students, says the simulators do more than provide practice for hooking up IVs and catheters. As a performance evaluator, it broadens their perspectives and makes them more self-reflective.
“Students gain a lot from that,” she says. “After going through it and applying all the didactic tools they are equipped with, they eventually say, ‘Oh, I’ve got it,’ or ‘I need to improve on that.’”
Sandra Allen, chair of undergraduate nursing studies, says the department integrated the simulations into health assessments for the first time over the summer semester. The feedback from students was glowing. They immensely enjoyed the physical interaction as an opportunity to apply the skills they learned in the classroom to a real-world situation.
“It really made them start feeling like they were nurses,” she says.
Although the simulators are valuable educational tools, assistant professor Sandra Davis says their impact extends far beyond the Brenau campus. Students who have experiences with the models require less orientation from employers when they make the leap from the classroom to real hospital and clinical settings.
“It benefits the facilities we are serving in this community,” she says. “You’re not going to have the lag-time of a new nurse who has not had a realistic experience learning how to do things.”
Demonstrable results
Andrea Gaines, a 2015 Brenau grad who now works at Habersham Medical Center, says the simulators definitely made an impact on her. She vividly recalled her first training exercise, in which her patient went into cardiopulmonary arrest.
“That was our first taste of how wrong something could go if we, as nurses, didn’t pay enough attention,” she says.
In addition to giving Gaines practice with head-to-toe assessments and inserting nasogastric tubes, the experiences taught her the critical importance of teamwork.
“It helped emphasize that nursing is not a solo profession,” she says. “We can pull from the different strengths of each person on the team. In doing that, we can treat the patient in the most effective way.”
Those in Brenau’s nursing programs, however, are not the only students who may benefit from the simulation lab. This fall, Brenau University will hold an interdisciplinary “tabletop exercise,” involving nursing, physical therapy, occupational therapy, psychology and pre-physician assistant students. Eventually, Hewett says she would like to bring all of them into the simulation lab for a group session, in which they have to use their diverse skill sets to draw up the best recovery plan for a patient. “Perhaps we could have a stroke victim, and everybody would come together and talk about their rehabilitative goals,” she says. “That would show how different professions have to work together for patient care.”
The simulators, Allen says, are just one aspect of the nursing department’s commitment to emerging healthcare technologies. In addition to those models, she says Brenau has also invested in IV pumps with medical library information built into them, mobile computer stations, barcoded medication systems and electronic medical records programs.
Getting nursing students acquainted and comfortable with such cutting-edge hardware and software, she says, is a necessity in an industry constantly being shaped and transformed by electronic innovations.
“Technology is truly a part of health care today,” she says. “We are working to integrate that into everything we are doing at Brenau.”